Motor Neurones, Resilience and Integrative Care
 The recent news of Grey’s Anatomy star Eric Dane’s death at the age of 53 following an ALS diagnosis has once again brought this rare neurological condition into public awareness. When a public figure faces such a diagnosis, it understandably prompts reflection: about vulnerability, about health and about what, if anything, we can meaningfully influence in our own lives.
The recent news of Grey’s Anatomy star Eric Dane’s death at the age of 53 following an ALS diagnosis has once again brought this rare neurological condition into public awareness. When a public figure faces such a diagnosis, it understandably prompts reflection: about vulnerability, about health and about what, if anything, we can meaningfully influence in our own lives.
Amyotrophic Lateral Sclerosis (ALS) is one form of motor neurone disease (MND). Motor neurones are specialised nerve cells responsible for carrying signals from the brain and spinal cord to our muscles. They allow us to move, speak, swallow and breathe. Upper motor neurones originate in the brain and send signals down through the spinal cord. Lower motor neurones extend from the spinal cord to the muscles. In ALS, both types progressively degenerate, leading to muscle weakness and loss of function.
There are other forms of motor neurone disease, including Primary Lateral Sclerosis (which primarily affects upper motor neurones), Progressive Muscular Atrophy (which mainly involves lower motor neurones), and Progressive Bulbar Palsy (which affects speech and swallowing). These conditions vary in presentation and progression, but all involve disruption to motor neurone signalling.
In approximately 90 to 95 per cent of ALS cases, the condition is described as sporadic. This means there is no clear family history and no single inherited mutation identified. Around 5 to 10 per cent are familial, linked to specific gene variants. Increasingly, research suggests that both genetic susceptibility and environmental influences may interact within a broader biological context. However, in most cases, a single definitive cause is not found.
ALS Is Not A Lifestyle Disease
It is important to state clearly that ALS is not considered a lifestyle disease. Most people living ordinary lives will never develop it. There is no credible evidence that routine stress, minor dietary imbalance or everyday musculoskeletal strain directly causes ALS.
At the same time, broader neurological health is influenced by the overall physiological environment of the body. Research continues to explore how chronic inflammation, oxidative stress, toxic exposure, repeated head trauma and metabolic dysfunction may contribute to vulnerability in some individuals. These factors are not causes in isolation, nor do they predict disease. They are part of a wider picture of systemic resilience.
Rather than asking whether we can prevent a rare condition, a more constructive question may be how we can support long-term neurological wellbeing in general.
- Avoiding smoking and vaping remains one of the clearest steps to protect vascular and neural health.
- Reducing prolonged exposure to pesticides, heavy metals and industrial solvents limits toxic burden.

- Maintaining metabolic stability: including healthy blood sugar regulation, appropriate body composition and cardiovascular fitness, supports mitochondrial energy production, which is fundamental to neuronal function.
- Moderate, regular physical activity improves circulation and overall health.
- Restorative sleep supports normal neural maintenance processes and metabolic waste clearance within the brain. Managing chronic stress and supporting emotional regulation may also help reduce sustained inflammatory load.
Supporting General Neuromusculoskeletal Health
The endocrine system plays an important regulatory role as well. Hormones influence metabolism, immune signalling and stress responses, all of which intersect with nervous system function. While medically supervised hormone therapy can be appropriate and beneficial, chronically pushing hormonal systems beyond physiological ranges, for example through unsupervised anabolic steroid use or extreme biohacking practices may disrupt metabolic and inflammatory balance. The aim in integrative care is not to override natural regulatory systems, but to support equilibrium.
Within this broader framework, holistic chiropractic and integrative care have a role, not in preventing ALS, but in supporting general neuromusculoskeletal health.
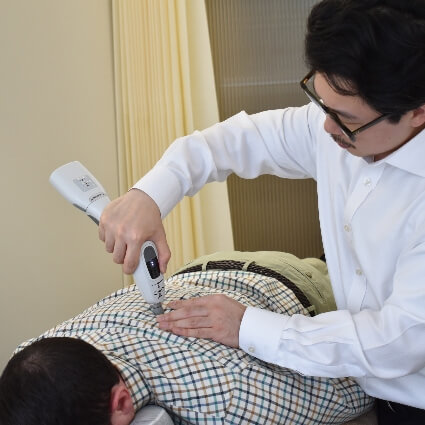 The spinal column houses and protects the spinal cord, which is central to motor signalling. Mechanical strain, persistent musculoskeletal tension and reduced movement variability can contribute to chronic discomfort and altered sensory input. Evidence supports that appropriate manual therapy, rehabilitation and movement retraining can reduce pain, improve functional mobility and support overall physical wellbeing.
The spinal column houses and protects the spinal cord, which is central to motor signalling. Mechanical strain, persistent musculoskeletal tension and reduced movement variability can contribute to chronic discomfort and altered sensory input. Evidence supports that appropriate manual therapy, rehabilitation and movement retraining can reduce pain, improve functional mobility and support overall physical wellbeing.
When delivered within an integrative model, combining manual care, movement rehabilitation, stress regulation and lifestyle guidance, the focus extends beyond symptom relief. The goal is to reduce cumulative physical strain, support healthy movement patterns and encourage sustainable self-care behaviours. While such care does not alter the underlying biology of motor neurone disease, it can meaningfully improve quality of life, physical comfort and overall resilience.
None of these measures offers certainty against rare neurological conditions. Medicine does not offer guarantees. However, cultivating metabolic balance, reducing toxic exposure, supporting physical function and maintaining regulatory stability represent sensible, evidence-aligned approaches to long-term health.
When high-profile diagnoses bring attention to conditions such as ALS, they remind us of human fragility. They can also remind us of the importance of caring for the systems that allow us to move, think and participate fully in life.
Responsible Care
In integrative practice, the emphasis is not solely on lifespan, but on healthspan: the capacity to live with ease, clarity and engagement. Supporting spinal health, metabolic balance and nervous system regulation is not about fear of disease. It is about stewardship of the body over time.
That is a goal grounded not in speculation, but in responsible care.