Neuroplasticity is one of the most important discoveries in modern neuroscience. It describes the nervous system’s ability to adapt, reorganise, and change in response to experience, injury, learning, and environment. Far from being fixed or static, the brain and nervous system remain adaptable throughout life.
Neuroplasticity is one of the most important discoveries in modern neuroscience. It describes the nervous system’s ability to adapt, reorganise, and change in response to experience, injury, learning, and environment. Far from being fixed or static, the brain and nervous system remain adaptable throughout life.
Although the term neuroplasticity is most commonly searched for in an educational context rather than as a treatment itself, understanding how it works helps explain why certain forms of care support recovery, resilience, and long-term function. It also provides a scientific framework for understanding how physical therapy, light-based therapies, and mindfulness-based approaches can influence healing.
Understanding Neuroplasticity
Neuroplasticity refers to the capacity of the nervous system to modify its structure and function. This includes strengthening or weakening neural connections, reorganising sensory and motor pathways, refining coordination, and adapting how the body responds to stress or pain.
These changes occur not only in the brain, but throughout the spinal cord and peripheral nervous system. Importantly, neuroplasticity can work in both helpful and unhelpful ways. While positive neuroplastic changes support recovery and improved function, maladaptive changes may contribute to persistent pain, stiffness, reduced confidence in movement, or heightened stress responses.
Effective healthcare aims to guide the nervous system toward healthier, more adaptive patterns, rather than simply masking symptoms.
Neuroplasticity, Pain, and Movement
 Pain is no longer understood as a purely structural or tissue-based issue. Contemporary pain science recognises that pain is shaped by the interaction of sensory input from the body, nervous system sensitivity, previous experiences, stress levels, sleep quality, and emotional context.
Pain is no longer understood as a purely structural or tissue-based issue. Contemporary pain science recognises that pain is shaped by the interaction of sensory input from the body, nervous system sensitivity, previous experiences, stress levels, sleep quality, and emotional context.
When pain becomes persistent, the nervous system may adopt an overly protective stance. This can lead to increased muscle tension, altered movement patterns, reduced coordination, and fear of movement. Over time, these changes can reinforce pain rather than resolve it.
Supporting neuroplasticity involves providing the nervous system with clear, calm, and meaningful input. This helps it reassess safety, restore movement options, and reduce unnecessary threat responses.
Chiropractic Care and Neuroplastic Change
Chiropractic care focuses on how joint movement, posture, and mechanical input influence the nervous system. Gentle spinal and joint adjustments provide precise sensory input through mechanoreceptors in joints and surrounding tissues. These receptors communicate directly with the nervous system and play a key role in movement control and body awareness.
Research suggests that this type of input can influence muscle tone, reflex activity, coordination, and pain processing pathways. Rather than forcing change, chiropractic care works by supporting neurological regulation and adaptive reorganisation.
Low-force techniques are particularly well suited to this approach, as they deliver meaningful input without excessive mechanical stress.
Activator Methods® and Precision-Based Care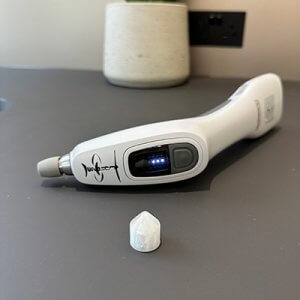
Activator Methods® Chiropractic Technique is a low-force, instrument-assisted approach that has been extensively studied. The Activator instrument delivers a rapid, controlled impulse with a force-time profile that closely matches an ideal sine wave. In simple terms, this means the force is delivered quickly, consistently, and precisely.
This precision allows the nervous system to receive a clear mechanical signal while minimising strain on joints and soft tissues. As a result, this approach is commonly used when a gentle, measured input is clinically appropriate, including in individuals seeking conservative and evidence-informed care.
Movement, Rehabilitation, and Neural Adaptation
Movement is one of the most powerful drivers of neuroplastic change. Functional rehabilitation and targeted exercise help retrain motor patterns, restore coordination, and improve balance and confidence.
When movement is introduced in a graded, appropriate way, it reinforces positive nervous system adaptation. This is particularly relevant for long-standing musculoskeletal issues, post-injury recovery, and post-surgical rehabilitation, where fear or avoidance of movement can slow progress.
Photobiomodulation and Nervous System Support
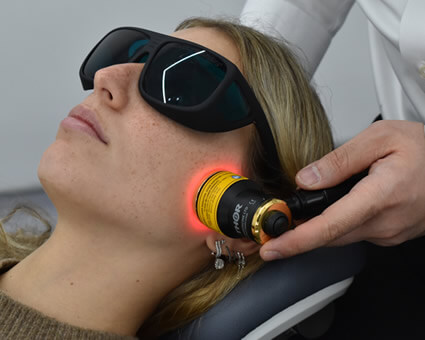 Photobiomodulation (PBM) therapy uses specific wavelengths of red and near-infrared light to support cellular and neurological function. Research has explored its effects on mitochondrial activity, inflammation modulation, nerve metabolism, and tissue recovery.
Photobiomodulation (PBM) therapy uses specific wavelengths of red and near-infrared light to support cellular and neurological function. Research has explored its effects on mitochondrial activity, inflammation modulation, nerve metabolism, and tissue recovery.
When applied clinically, PBM may help create physiological conditions that support neural adaptation and recovery. Interest has also grown in brain-directed PBM approaches, including transcranial and intranasal applications, which are being studied for their potential effects on cognitive function, mood regulation, and neurological rehabilitation.
This growing interest is reflected in search trends for treatments such as transcranial magnetic stimulation (TMS), particularly in major cities. While TMS is one approach used in specialist medical settings, PBM represents another non-invasive modality with an expanding research base in neurological health.
Mindfulness, Attention, and Neural Regulation
Neuroplasticity is influenced not only by physical input, but also by attention and awareness. Mindfulness-based practices have been shown to affect how the brain processes sensation, stress, and emotional responses.
By improving nervous system regulation, mindfulness can support changes in pain perception, reduce stress-driven muscle tension, and enhance the effectiveness of physical therapies. When combined with movement-based and manual approaches, it helps create a more stable foundation for long-term adaptation.
An Integrative Perspective on Recovery
Neuroplasticity does not respond to a single intervention. It responds to consistent, meaningful input across multiple systems. Integrating gentle chiropractic care, functional movement rehabilitation, clinical photobiomodulation therapy, and mindfulness-based approaches reflects a modern biopsychosocial understanding of health.
This integrated approach recognises that recovery is shaped by mechanical, neurological, and behavioural factors working together, rather than in isolation.
Why Neuroplasticity Matters in Care
Understanding neuroplasticity helps explain why recovery often takes time, why consistency matters more than force, and why addressing stress, movement confidence, and awareness can influence physical outcomes.
Rather than pursuing short-term fixes, neuroplasticity-informed care focuses on building resilience, adaptability, and sustainable function.
Neuroplasticity is not a treatment in itself, it is a biological process. The role of healthcare is to support that process by creating the right conditions for adaptation to occur safely and effectively.
Through evidence-informed chiropractic care and integrative therapies, it is possible to support the nervous system’s remarkable capacity to change, helping patients not only recover, but move forward with greater confidence, stability, and wellbeing.